 Diabetes is a disease that causes the body to be less responsive to insulin, a hormone that allows blood glucose (blood sugar) to enter cells and be used for energy. There are two main types of diabetes:
Diabetes is a disease that causes the body to be less responsive to insulin, a hormone that allows blood glucose (blood sugar) to enter cells and be used for energy. There are two main types of diabetes:
Type 1 or insulin dependent: This usually occurs during childhood or adolescence. The body cannot produce the amount of insulin required for its daily needs.
Type 2 or non insulin dependent: This is the most common form of the disease, which usually occurs after age 45. The body produces insulin, but the cells are resistant to it.
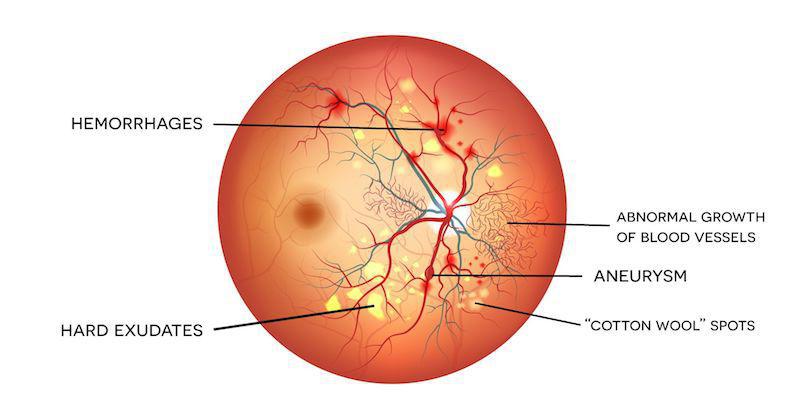
Diabetes is the number one cause of blindness in the United States in those 20-64 years old. Glaucoma, cataract, and corneal disease are more common in people with diabetes and contribute to their high rate of blindness. However, the major cause of blindness in people with diabetes is diabetic retinopathy. Diabetic retinopathy is a term used for all the abnormalities of the small blood vessels of the retina caused by diabetes, such as weakening of blood vessel walls or leakage from blood vessels. If not managed properly, retinopathy can progress from non-proliferative to proliferative.
 Non-proliferative retinopathy: This is a common, usually mild form of retinopathy that generally does not interfere with vision. Abnormalities are limited to the retina and usually will only interfere with vision if they involve the macula, the area on the retina that gives us the sharpest vision. If left untreated it can progress to proliferative retinopathy.
Non-proliferative retinopathy: This is a common, usually mild form of retinopathy that generally does not interfere with vision. Abnormalities are limited to the retina and usually will only interfere with vision if they involve the macula, the area on the retina that gives us the sharpest vision. If left untreated it can progress to proliferative retinopathy.
Proliferative retinopathy: This is the more serious form. It occurs when new blood vessels branch out around the retina. It can cause bleeding in the eye or detachment of the retina, and lead to blindness.
The key to preventing diabetic related eye problems is good control of blood sugar levels, a healthy diet and good eye care. Several studies such as the Diabetic Control and Complication Trial (DCCT) and the United Kingdom Progression of Diabetes Study (UKPDS) showed that strict blood sugar control limited both the onset and progression of diabetic retinopathy. In addition to this, blood pressure and cholesterol levels have to be controlled. Smokers should stop smoking, and overweight people with diabetes should develop a diet and exercise regimen to help them achieve a healthy weight.
Because a person with diabetes can have retinopathy and not know it, a regular checkup with an eye care professional is essential. Regular checkups with an eye doctor can detect retinopathy early and possibly prevent blindness.
What are my treatment options?
People with type 1 diabetes should see their eye care professional annually for a dilated eye examination beginning five years after the onset of diabetes.
Women with type 1 diabetes who are pregnant should have a comprehensive eye examination in the first trimester and close follow-up throughout pregnancy.
People with type 2 diabetes should see their eye care professional for a dilated eye examination shortly after diagnosis of diabetes and annually thereafter.
In mild cases, treatment for diabetic retinopathy is usually not necessary and monitoring is all that is required. In more advanced cases, treatment is recommended to stop the progression of diabetic retinopathy and prevent vision loss. Several treatment options are available under the guidance of a trained ophthalmologist.
Laser surgery: Laser light is focused on the retina in order to stimulate it and promote absorption of the surrounding fluid and reduce macular edema. For proliferative retinopathy, the laser treatments are delivered over the peripheral retina. The small laser scars that result will reduce abnormal blood vessel growth and swelling. Laser surgery may be performed in your ophthalmologist's office or in an out-patient setting.
Intraocular Injection: This is a newly emerging treatment for diabetic macular edema and neovascularization. This therapy helps to decrease the stimulus released by the retina for new vessel growth. It may also reduce the amount of fluid leaking into the retina, resulting in visual improvement. Due to the chronic nature of diabetic eye disease, this treatment may need to be repeated or combined with laser therapy to obtain maximal or lasting effect.
Vitrectomy: This surgery is recommended for advanced proliferative diabetic retinopathy. It removes any blood in the back of the eye and replaces it with clear fluid. Vitrectomy repair may also be necessary if scar tissue has detached the retina from the back of the eye. This microsurgical procedure is performed in the operating room by a trained vitreoretinal surgeon.